A Guide Specializing in the “Toxic effects” of todays battle field for all veterans who was deployed since August 1990.
Email Us Your Questions
NGWRC is funded only by donations
NGWRC is a 501(c)3 non-profit organization, and your donations are tax deductible. Our paperwork is on file with the state of Kansas and if you need a copy you can get it from the Secretary of States' office. The NGWRC reserves the right to refuse donations from any groups or persons whos' views does not support ours.
The History of the Gulf War Illness Act
a. On November 2, 1994, Congress enacted the “Persian Gulf War Veterans’ Benefits Act,” Title I of the “Veterans’ Benefits Improvements Act of 1994,” Public Law (PL) 103-446. After VA research showed that over 17,000 veterans on the Gulf War Registry exams were suffering from undiagnosed symptoms, many grass root groups worked to get Congress to help the Desert Storm veterans. The statute added a new section, 38 U.S.C. §1117, authorizing the Department of Veterans Affairs (VA) to compensate any Gulf War (GW) veteran suffering from a chronic disability resulting from an undiagnosed illness or combination of undiagnosed illnesses which manifested either during active duty in the Southwest Asia theater of operations during the GW, or to a degree of 10 percent more within two years following service in the Southwest Asia theater of operations during the Gulf War.
[Something that must be remembered is that this first passage of the law had a presumptive time of two years from the date that a servicemember left Southwest Asia. Many Gulf War veterans did not start to seek/complain of their illnesses until the mid-1990s. That was after the two-year time limit expired, and while many may have had what it took for filing their claims, the Veterans Benefit Administration (VBA) did not accept many of the claims, as per the law. Most of this was because the law was new and adjudicators did not understand it themselves. Those claims were denied on the basis of not being in the presumptive window. Many others were denied because evidence was not in their service records - something used to this date.]
b. The “Persian Gulf War Veterans’ Act of 1998,” PL 105-277, authorized VA to compensate GW veterans for diagnosed or undiagnosed disabilities that are determined by VA regulation to warrant a presumption of service connection based on a positive association with exposure to one of the following as a result of GW service:
- a toxic agent
- an environmental or wartime hazard, or
- a preventive medication or vaccine
Note: This statute added 38 U.S.C. 1118. For the purposes of this regulation, a Persian Gulf veteran means a veteran who served in the active military, naval, or air service in the Southwest Asia theater of operations during the Persian Gulf War, which by law runs from August 2, 1990 through a date yet to be determined by law or Presidential proclamation (38 U.S.C. 101(33)). The Southwest Asia theater of operations is defined according to Executive Order 12744 of January 21, 1991, in which President Bush designated the combat zone of the Persian Gulf War, and includes Iraq, Kuwait, Saudi Arabia, the neutral zone between Iraq and Saudi Arabia, Bahrain, Qatar, the United Arab Emirates, Oman, the Gulf of Aden, the Gulf of Oman, the Persian Gulf, the Arabian Sea, the Red Sea, and the airspace above these locations.
The 1998 change made service a presumption when it established the end-date and §1118. This meant a servicemember no longer had to have proof in his or her records for two years from leaving the desert. The §1118 meant a nexus was not needed as per the meaning of presumption of service. However, the VBA still did a large number of these claims incorrectly and did deny them for not having a diagnosis and or a nexus. There are two court cases on the nexus that the VBA subsequently lost. This meant the requirement for “service connection based on a positive association with exposure” nexus was not legal.
c. The “Veterans Education and Benefits Expansion Act of 2001,” PL 107-103, expanded the presumption part for GWI with the definition of “qualifying chronic disability” under 38 U.S.C. §1117 to include, effective March 2002, not only a disability resulting from an undiagnosed illness but also:
- a medically unexplained chronic multi-symptom illness that is defined by a cluster of signs and symptoms, and
- any diagnosed illness that is determined by VA regulation to warrant presumption of service connection
- The Secretary added chronic fatigue syndrome, fibromyalgia, and irritable bowel syndrome as presumptive illness under 38 CFR §3.317 as seen in the Federal Register of June 10, 2003.
d. July 2010 change - 38 CFR §3.317, which implements 38 U.S.C. §1117, defined GW service and “qualifying chronic disability,” and provided:
- a broad, but non-exclusive, list of signs and symptoms which may be representative of undiagnosed or chronic, multi-symptom illnesses for which compensation may be paid,
- and the presumptive period for service connection
Qualifying chronic disability, under 38 CFR §3.317, means a chronic disability resulting from any of the following or any combination of the following:
- an undiagnosed illness
- a medically unexplained chronic multi-symptom illness, such as chronic fatigue syndrome, fibromyalgia, and irritable bowel syndrome, that is defined by a cluster of signs or symptoms (There are some rule changes that will help the veterans in this area.) and/or
- any diagnosed illness that is determined by VA regulation to warrant a presumption of service connection
e. November 2011 change = the presumptive period for manifestation of qualifying chronic disability under 38 CFR §3.317
- begins on the date following last performance of active military, naval, or air service in the Southwest Asia theater of operations during the GW,
- and extends through December 31, 2021
38 CFR §3.317 specifies the following thirteen categories of signs or symptoms that may represent a qualifying chronic presumptive disability. The list of thirteen symptom categories is not exclusive.
• undiagnosed abnormal weight loss |
• undiagnosed menstrual disorders |
• undiagnosed cardiovascular signs or symptoms |
• undiagnosed muscle pain |
• undiagnosed fatigue |
• undiagnosed sleep disturbances |
• undiagnosed gastrointestinal signs or symptoms |
• undiagnosed neurologic signs or symptoms |
• undiagnosed headache |
• undiagnosed neuropsychological signs or symptoms |
• undiagnosed joint pain |
• undiagnosed signs or symptoms of the skin |
• undiagnosed signs or symptoms involving the upper respiratory system |
• undiagnosed signs or symptoms involving the lower respiratory system |
Signs or symptoms not represented by one of the listed categories may also qualify for consideration under 38 CFR §3.317.
To qualify, the claimed disability must be chronic, that is, it must have persisted for a period of six months or more. A claimant must measure the six-month period of chronicity from the earliest date on which all pertinent evidence establishes that the signs or symptoms of the disability first became manifest.
Note: If a disability is subject to intermittent episodes of improvement and worsening within a six-month period, consider the disability to be chronic.
f. July 2010, a letter was sent to all of the adjudicators with a revision to 38 C.F.R. § 3.317 to clarify the Meaning of “Medically Unexplained Chronic Multisystem Illness” Related to Gulf War and Southwest Asia Service. VA is revising 38 C.F.R. §3.317 to clarify that the three listed, diagnosed multi-symptom illnesses are not exclusive, but rather are examples that can serve to inform VA medical examiners and adjudicators of the general types of medically unexplained chronic multi-symptom illnesses that may qualify for service connection under the 38 U.S.C §1117 authority.
What is Gulf War Service (1990-current*)
 Only someone
deployed to the area of operation is a `Gulf War Veteran' and may file §3.317(a)
claims. A Persian Gulf Veteran is any current or former member of the United
States Armed Forces who served in the Southwest Asia Theater of Operations for
at least one day between August 2, 1990 and the current date*. This includes,
but is not limited to, serving in Operation Desert Shield, Operation Desert
Storm, Operation Iraqi Freedom, and Operation New Dawn (Iraq Theater).
Only someone
deployed to the area of operation is a `Gulf War Veteran' and may file §3.317(a)
claims. A Persian Gulf Veteran is any current or former member of the United
States Armed Forces who served in the Southwest Asia Theater of Operations for
at least one day between August 2, 1990 and the current date*. This includes,
but is not limited to, serving in Operation Desert Shield, Operation Desert
Storm, Operation Iraqi Freedom, and Operation New Dawn (Iraq Theater).
*See: http://www.publichealth.va.gov/exposures/gulfwar/military-service.asp
The end date of the presumed period is established by Congress. Current regulation ends it on December 31, 2021.
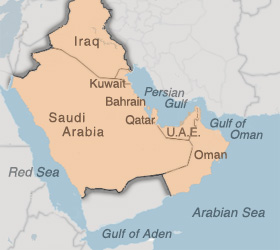
Congress has defined the Southwest Asia Theater (SWAT) of Operations as:
· Iraq · Kuwait · Saudi Arabia · Bahrain · Qatar · The neutral zone between Iraq and Saudi Arabia |
· Oman · The United Arab Emirates (U.A.E.) · Gulf of Aden · Gulf of Oman · Waters of the Persian Gulf, the Arabian Sea, and the Red Sea · The airspace above these locations
|
A servicemember must meet these time and location criteria in order to receive service-connected status under §3.317.
If someone has a medically unexplained chronic multi-symptom illness or similar illness which they believe is service-connected, but they do not meet the definition of a Gulf War Veteran as Congress defines it, they may still file a claim, but the claim will not fall under 38CFR§3.317. Such a claim could be filed under other regulation, like §§ 3.303, 3.304(b), 3.307, and it will have a different burden of proof.
Where is the current regulation posted and how do I use it?
The VBA does not use the M21-1MR anymore, so if you see someone using it, it has been out of date since 2016. Use the link here, as it will take you to the VA “live manual.” Go to: http://www.knowva.ebenefits.va.gov/ and enter one of the terms ‘Undiagnosed, Fibromyalgia, or IBS’ in the search engine. It will bring up some help sections for you. Use this to see what you need to build your claim. Work with your Veteran Service Organization representative to ensure you are not adding information that is not in the file or that may harm your claim. You can also Google “38 CFR §3.317” to see what is on the internet. Something like “The DoD is covering up what happened---“and a blog on it will harm your claim.
These regulations change frequently. You should download the regulation in effect when you first file. Make a second copy and give it to your VSO representative with your other documentation, unless you have a representative who already specializes in Persian Gulf Claims. We have seen outdated regulations used in the decisions of veteran’s claims, and this does make for an error.
What is Gulf War Illness and who may file a claim for it?
Gulf War Illness (GWI) is only a term and cannot be used when filing for a claim under 38 CFR §3.317. If someone files a claim by saying, “I am filing for Gulf War Illness due to my service,” the Regional Office will send a letter asking what symptoms are being considered. This is where many doctors, the WRIISC, and some veterans pushing for change get it wrong. The law does not have any term of GWI in it, nor is there an IC10 code for it. If a doctor diagnoses someone with GWI, just what is he saying? Without the doctor spelling out the symptoms and testing to rule out the other types of illness, be ready for the long haul.
GWI is a term that refers to the listed symptoms first documented among the veterans of Operation Desert Storm as they returned home in 1991. More than one in four of these veterans are estimated to experience a wide range of unexplained symptoms or a CMI - such as fatigue, pain, and problems with digestion - for which there is no visible cause or explanation. Many have had these conditions since their deployment or soon after their return home. Still others became ill later in their lives.
It took years of strong advocacy by veterans and the NGWRC before much of the medical community, including the VA, accepted GWI as a medical disorder. Today, the exact cause remains unknown and treatment is still far off. Scientific research proves that whatever the cause, the disability is real and it is likely related to military service in the Persian Gulf region. Treatment methods and compensation ratings for this condition are still evolving.
The Institute of Medicine (IOM) said in 2013 to use the term “Gulf War Illness” (GWI) to refer to the symptoms and illnesses that apply to all GW-veterans affected by the disorder. Exposures present in the Southwest Asia Theater (SWAT) of Operations greatly increased the risk of GWI among Gulf War Veterans. This distinction is for medical research and not, as advised above, for filing claims with the VBA. GWI remains a descriptive medical term. To date there is not even a case definition. The VA is working on a clinical case definition, and the NGWRC is a part of those talks. Even after there is a new clinical case definition, it would need to be tested and checked out by the National Academy of Science. Then the VBA would need to change the regulation. Then Congress might have to even change the law.
In the rest of this guide, we will refer to definitions and symptoms based on federal law, court cases, and VA regulations and guidelines, even if they are not updated to reflect the most recent scientific research. A claim is based on the laws and regulations as well as the court cases. A large study may help in a claim when it comes to the benefit of the doubt, but a pilot study will not. Unfortunately, most Gulf War studies are pilot studies. The VA has done some large studies that can help, but like everything else, a claimant still needs a nexus with it. Veterans cannot give the nexus that comes from a doctor in a given field.
When an Iraq or Persian Gulf veteran files a claim for compensation related to GWI/CMI, he or she is filing for presumptive service-connection of a qualifying chronic disability in accordance with laws and regulations. Qualifying chronic disability, under 38CFR§3.317(a)(2)(i), means a chronic disability resulting from any of the following or any combination of the following:
(A) An undiagnosed illness;
(B) A medically unexplained chronic multi-symptom illness that is defined by a cluster of signs or symptoms, such as:
1. Chronic fatigue syndrome (CFS)
2. Fibromyalgia (FM)
3. Functional Gastrointestinal Disorders (FGID) (excluding structural gastrointestinal diseases)
In summary, the law passed by Congress only allows those with what we generically call “Gulf War Illness” to receive compensation for their symptoms or for a diagnosed medically unexplained chronic multi-system illness. Veterans who file for only “Gulf War Illness” will get a letter from their VARO asking them to clearly define just what symptoms they are claiming. When filing, use this guide and do it right. The VA grants presumptive service-connection to Gulf War Veterans for Medically Unexplained Chronic Multisystem Illness which are rated at least 10% disabling, and which manifest the disabling symptoms for at least six consecutive months before the end of 2021. It does not matter whether the Medically Unexplained Chronic Multisystem Illness is one of the diagnoses named in §3.317(a)(2)(i)(B). The change to the regulation found in the VA’s fast letter FL 10-26 sent out July 21, 2010 explains that they are examples.
Chapter II will explain undiagnosed illness claims (UDX), and we will cover the other parts of the regulation in other chapters.
When you became injured in the line of duty[4], you might earn treatment and compensation for that injury. However, you still have to prove that (1) your injury occurred, (2) it is currently disabling, and (3) it is connected to your service. Among veterans, as in the civilian world, a small number of individuals make false claims while others make honest but erroneous claims. The VA, therefore, must perform its due diligence before a claim is completed.
On the VBA side, some adjudicators do not understand injuries like PTSD, TBI, and GWI/UMCMI. These factors combine to create a complex claims adjudication system which places a heavy burden on veterans. This guide is to help you to better understand “undiagnosed illness” and “medically unexplained chronic multi-symptom illness.” We hope that you learn to build any claim -- with the facts you need – in order to increase the likelihood that you will prevail on your claim or appeal.
No matter what condition or injury you live with as a result of your service, you have the burden of proof to meet before the VA will grant the benefits you are seeking. You are in effect suing the government for the injuries that happened to you while you were in the service. At the same time, you will not be able to make a claim for everything that happened to you.
The VA is required to consider all evidence of record and to consider, and discuss in its decision, all potentially applicable provisions of law and regulation. See Schafrath v. Derwinski, 1 Vet.App. 589 (1991); Weaver v. Principi, 14 Vet. App. 301, 302 (2001). When the VA fails to do so, it is an error in your claim.
The VA must also give a statement that is adequate to enable a claimant to understand the precise basis for the decision. See 38 U.S.C. 7104(d)(1); Allday v. Brown, 7 Vet. App. 517, 527 (1995); Simon v. Derwinski, 2 Vet.App. 621, 622 (1992).
There are five different ways for you to be granted benefits from the VA, but this guide will only look at three: Direct, Secondary, and Presumptive. Specifics for each follow.
A Claim for Direct Service Connection
It should be noted that this is the only one of the five means for service connection where a veteran most likely will need to show something in the Service Treatment Records (STR). In a proper Gulf War presumptive claim a veteran does not need any proof in the STR.
For a claim of direct service connection, you will need the following:
1. Medical evidence of a current disability,
2. Medical evidence, or in certain circumstances, lay evidence of an in-service incurrence or aggravation of a disease or injury;
3. Medical evidence of a nexus between the claimed in-service disease or injury and the present disease or injury.
The regulations for a direct service connection are 38 CFR 3.303 and 38CFR §3.304. As §3.303(d) states “Post-service initial diagnosis of disease. Service connection may be granted for any disease diagnosed after discharge, when all the evidence, including that pertinent to service, establishes that the disease was incurred in service.”
There are times the VBA forgets about some of the parts of 38 CFR §3.303(b), such as this part:
Continuity of symptomatology is required only where the condition noted during service (or in the presumptive period) is not, in fact, shown to be chronic or where the diagnosis of chronicity may be legitimately questioned. When the fact of chronicity in service is not adequately supported, then a showing of continuity after discharge is required to support the claim.
Most claims will be denied for not being chronic, so you still show the continuance of symptomatology after service until a diagnosis is rendered. The claim should then be granted. If denied, file the appeal and the evidence to show this. Remember symptoms are not in the service then again 20 years later; they are ever since service.
TopA Claim for Secondary Service Connection
These claims fall under 38 C.F.R. § 3.310(b). You need to prove that a secondary condition was caused or aggravated by your service-connected condition. When this includes the treatment for your service-connected condition, you need to so state it. Then you may raise the issue of aggravation by the rated issue and all other rated issues -- as well as the treatment given. The VA will look at the combined medical file. See El-Amin v. Shinseki, 26 Vet. App. 136, 140-41 (2013). You do have to lay it out better than this.
In a claim for secondary service connection, you first need a diagnosis of an illness or injury, just as you do for a direct connection. You will then need a medical nexus with a very good rationale that provides a link between that diagnosis and the issue that you do have rated by the VA. This nexus needs to come from a doctor who knows the particular medical area. A psychiatrist, for example, cannot give a nexus between your service connected knee injuries and a subsequent, secondary hip problem. An orthopedic surgeon would have a more medically legitimate position in this case. The psychiatrist, however, can prepare a nexus statement on how mental health medications can cause erectile dysfunction (ED), weight gain, or high blood pressure. Remember that you or your doctor need to give the research reference/ papers with your claim, too. These nexus assessments can be notes in your medical files with a letter you send in to the VBA from your doctor.
A Claim for Presumptive Service Connection
Presumptive service connection is addressed in different sections of the CFR, like §3.307, §3.309, §3.317 and §3.318. Claims in this category are the easiest to assess, because the VA has already determined that if a veteran has certain symptoms/conditions, they are presumed to stem from service in that area of operations during the deployed period. In other words, if a servicemember’s time and geographical requirements are met, the VA presumes service connection if he or she has a particular affliction. The elements are the same, and you must meet the requirements in that section of the regulation for that type of presumptive connection. If you do not meet the allocated window/dates of service, are outside the timeframe set for the symptoms to first show, or have something happen to cause the same symptom after you left the area of combat as in 38 U.S.C. §1113, then you cannot use the presumptive connection. All presumptives must be able to be rated at 10% or more before the VBA will grant them.
For presumption of service connection from case law on Gulf War claims, see Gutierrez v. Principi, 19 Vet.App. 1 (2004). In order to establish service connection under 38 U.S.C. §1117 and 38 C.F.R. §3.317, a claimant must present evidence that he or she is a Persian Gulf veteran who (1) exhibits objective indications; (2) of a chronic disability such as those listed in paragraph (b) of 38 C.F.R. §3.317; (3) which became manifest either during active military, naval, or air service in the Southwest Asia theater of operations during the Persian Gulf War, or to a degree of 10% or more not later than December 31, (2021); and (4) such symptomatology by history, physical examination, and laboratory tests cannot be attributed to any known clinical diagnosis.
Most claims will get denied without these factors, and then you would need to file a Notice of Disagreement (NOD). You need to make sure to use the VBA’s new form when doing this. You can read more on this in the Claims 101 section.
TopThe Perspective of a Doctor
Before going to the next chapter, here is some advice, born from experience, on VA medical personnel. Doctors are professionals, and you need to treat them as such. You did not treat the doctors in the service with disrespect, so do not treat your non-military doctors with disrespect.
Your VA doctors do not have your military medical files, so they cannot make a nexus statement to your service. They will prepare medical notes and diagnoses from post-service conditions. Moreover, VA doctors can only see what is in your health records on the VA computer system (from your visits to the VHA). Your service medical records or STR are in your claims file, a legal file at the Veterans Benefits Administration (VBA). Only the C&P examiner will get to see the STR for your C&P. There are ongoing initiatives to merge active duty and VA medical records, but that is not in place now.
This limited access does keep your doctors from knowing what happened to you in the service, so he/she is starting off cold. You may get upset if many tests are redone, especially if you had these tests done just months before. In addition, many veterans who visit the WRIISC will find that researchers may be skeptical, as they, too, cannot see the military records to determine when an illness started. As Desert Storm veterans, we have years of hand-written or paper files, and only a few have been transcribed for someone to search in a computer program. That said, many servicemember’s are provided with paper copies of their medical records at the time of their separation, and these could be useful to a physician or researcher.
Even if you feel frustrated, being disrespectful toward your doctor will not be in your interest. Keep in mind that if you “go off” on a doctor in a non-VA hospital, you may find yourself in jail; in the VA, you can find yourself with U.S. marshals leading you to your appointments. If you want to be treated well, treat others the same way.
The doctor’s job is to find out what is causing the symptoms in your body today and to determine the best treatments to relieve those symptoms. As you work with him, focus on what he needs to know to help you now. This is where your medical journal, ‘Gulf War Review,’ and large VA studies (not the CDRMP or any other pilot studies) will come into play.
When you are giving your doctor information about your medical condition, focus on information related directly to it. What symptoms do you have now? How severe are they? How do they affect your work and other daily activities? When did they begin? Have they gotten worse or better over time? Does this doctor have full access to your medical records, or do you need to obtain copies of some records and bring them to him or her? Do they know about the WRIISC? Ask about getting help from the WRIISC. Give the doctor a WRIISC handout that is on the NGWRC website or google the WRIISC and print out the VA page to take to them.
If you go beyond this and begin focusing on specific events that you think caused the condition, or on how you believe you were wrongly ignored or improperly treated in the past, you could end up with a referral for mental health treatment instead of the medical care and diagnoses you need to manage your disability.
You cannot diagnose yourself with any of the conditions in this guide. Only a doctor can diagnose conditions, NOT a nurse-practitioner or physician’s assistant (PA). The appeal of the claim will not hold up unless medical documentation comes from a doctor. It is best if the doctor that did diagnose you is an expert in the field of that illness. Submit paperwork to show the doctor is an expert if you use a non-government doctor.
If you, as a veteran, encounter difficulties at a VA medical facility, you may contact the patient advocate at that location for assistance in resolving the problem. If that does not work, you may move up the ladder until you get the help you need. In some cases, you may be assigned a doctor who does not understand your injury or who is unwilling or unable to help you. If so, the social worker (or patient advocate) is there to help you get things worked out. Your team social worker and the patient advocate can even help you get a different doctor. Do not suffer with a doctor that will not help you.
If you are using a Community-Based Outpatient Clinic (CBOC), you may have to go to a VA Medical Center to see a different doctor who has expertise in your situation. A CBOC may not have enough flexibility or staff to change your Primary Care Provider. Many of the VA CBOCs use PAs or nurse-practitioners, and a doctor may not be available. In this case, you will need to find someone else, either at the medical center or, if authorized, a civilian doctor with the appropriate specialty.
Finally, a short review of the VA’s structure. The VA is a Department which has three principal subordinate elements called administrations. The National Cemetery Administration (NCA), as the name implies, is responsible for federal cemeteries world-wide. The Veterans Health Administration (VHA) is the medical component of the VA. For our purposes here, the VHA is the system of hospitals, clinics, doctors and other medical staff, and research where the veteran goes for medical assessment and treatment. The Veterans Benefit Administration (VBA) is responsible for assessing and providing benefits to eligible veterans (which includes acting upon records provided by VHA doctors). These benefits include educational and home loan assistance, but our concern here is with the VBA’s role in reviewing and providing disability benefits for those afflicted with GWI symptoms. This work is performed in a VA Regional Office by personnel trained to advise upon, review, and adjudicate a claim. The VBA is also the VA component in the event the veteran appeals the initial decision.
Top
[1] We are using Gulf War Illness only as the term for what Congress has passed into law in 1994 and updated in 2001. As per the law, there is no place to file a claim for Gulf War Illness. You file for the symptom in part (a) or the CMI’s as in part (b).
[2] We are using Gulf War Illness only as the term for what Congress has passed into law in 1994 and updated in 2001. Per the law, there is no place to file a claim for Gulf War Illness. You file for the symptom(s) in part (a) or the CMI’s as in part (b).
[3] For our purposes, a SWA veteran is anyone who has served in Operations Desert Shield/Storm, Cease Fire Operations, Operation Southern Watch, Operation Iraqi Freedom (OIF), Operation New Dawn (OND), Operation Enduring Freedom (OEF), and any others which may occur. This is more than just the Gulf War subset.
[4] In line of duty means an injury or disease incurred or aggravated during a period of active military, naval, or air service unless such injury or disease was the result of the veteran's own willful misconduct or, for claims filed after October 31, 1990, was a result of his or her abuse of alcohol or drugs. Authority: 38 U.S.C. §105


